Obesity is a complex chronic disease that is growing worldwide and affects approximately 1/3 of the adult population in Portugal. Gastroesophageal reflux disease (GERD) is also highly prevalent, affecting approximately 20% of the population.
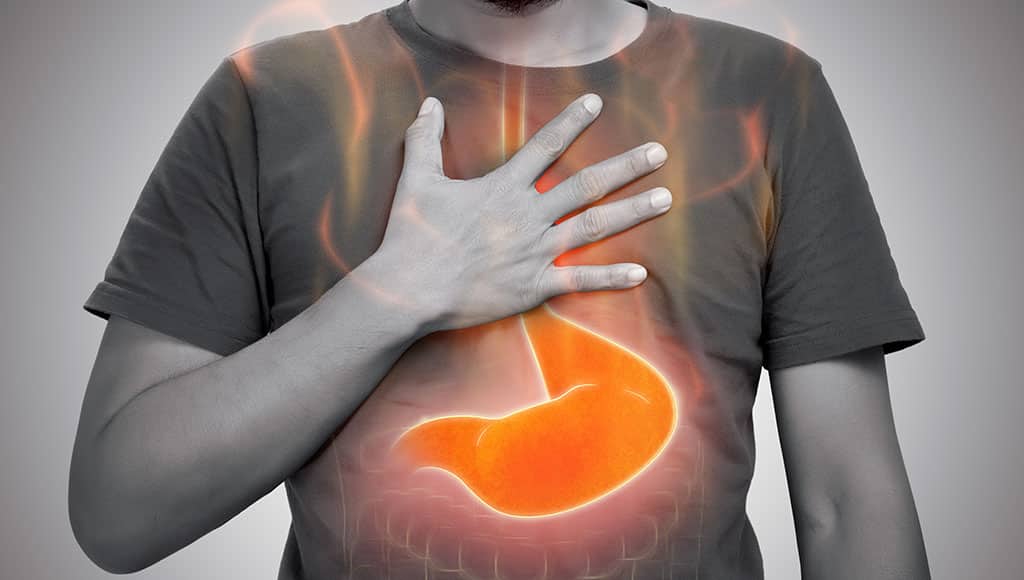
GERD is a digestive condition characterised by the return of gastric contents to the oesophagus, causing symptoms such as heartburn, regurgitation, chest pain and, in more severe cases, oesophageal inflammation or lesions. In recent years, several studies have demonstrated a clear association between the increase in obesity rates and the incidence of GERD, suggesting that excess body weight may be a significant risk factor for the development and worsening of this disease.
Obesity, especially abdominal obesity (central obesity), contributes to increased intra-abdominal pressure. This additional pressure makes it difficult for the lower oesophageal sphincter, the valve that prevents stomach contents from flowing back into the oesophagus, to function properly.
When this valve weakens or relaxes inappropriately, reflux becomes more frequent. In addition, excess adipose tissue, particularly visceral tissue, can alter the normal anatomy of the gastrointestinal tract, favouring conditions such as hiatal hernia, which is closely linked to GERD.
Clinical and epidemiological studies reinforce this connection. Obese patients have a two to three times greater risk of developing reflux compared to individuals of normal weight. In addition, there is a dose-response relationship: the higher the body mass index (BMI), the greater the frequency and severity of GERD symptoms. This correlation is observed in both adults and children, which makes obesity a concern from childhood.
Another relevant aspect is that obesity can compromise the response to GERD treatment. In many cases, medications used, such as proton pump inhibitors, are less effective in overweight patients. In these individuals, symptom control may require higher doses or complementary therapies. On the other hand, weight loss has been shown to be an effective intervention both in reducing symptoms and in preventing disease progression. Studies indicate that even a small loss of 5% to 10% of body weight can result in significant improvements in the frequency and intensity of reflux.
Treatment of GERD in obese patients, therefore, must go beyond the pharmacological approach. Lifestyle changes are essential. In addition to weight loss, it is recommended to avoid foods that promote relaxation of the lower oesophageal sphincter, such as fatty foods, fried foods, chocolate, caffeinated beverages and alcohol. It is also advisable to avoid large meals, especially before bedtime, elevate the head of the bed and stop smoking.
In short, obesity plays a central role in the development and maintenance of gastroesophageal reflux disease. Recognizing this association is essential not only for a more accurate diagnosis but also for the development of more effective and long-lasting therapeutic strategies. The integration of clinical measures and lifestyle changes, especially weight control, represents a fundamental step in promoting gastrointestinal health and preventing complications associated with GERD.
Article submitted by the HPA Group