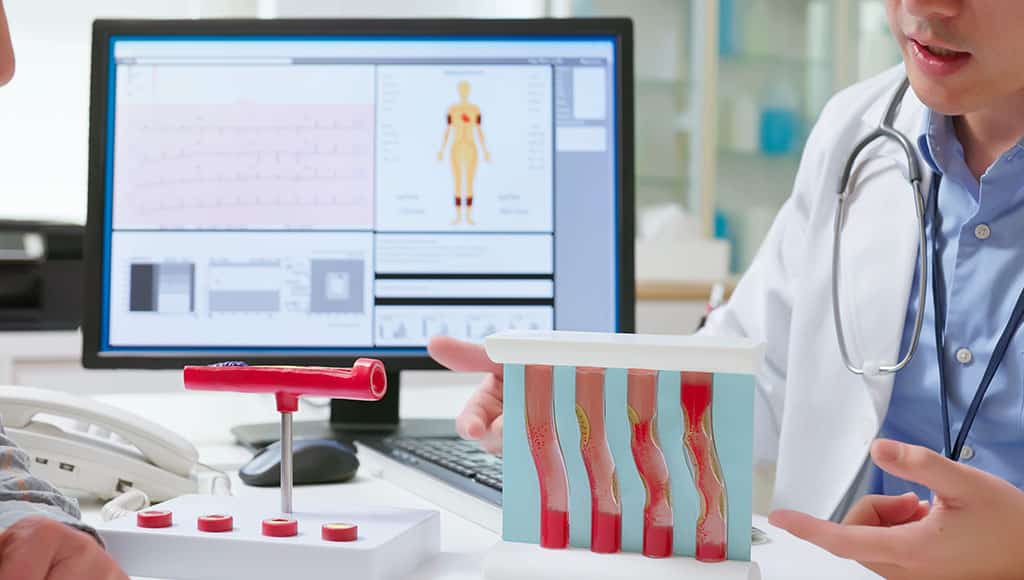
Although traditionally associated with physical factors such as hypertension, diabetes, smoking, and high cholesterol, recent studies have demonstrated a strong link between mental health and cardiovascular disease, especially atherosclerosis.
Mental illnesses such as depression, chronic anxiety, schizophrenia, and bipolar disorder are more than just emotional imbalances. They affect the body as a whole, including the cardiovascular system. Several studies have shown that people with mental disorders have a higher risk of developing atherosclerosis and its complications, even after adjusting for other known risk factors.
But how exactly does the mind influence the heart and blood vessels?
First, there are biological mechanisms. Mental illness, especially when untreated, is associated with high levels of chronic stress. This state constantly activates the hypothalamic-pituitary-adrenal axis, leading to the excessive release of cortisol, a hormone that, at prolonged high levels, promotes inflammatory processes and changes in lipid metabolism. This contributes to the development and progression of atherosclerosis.
Furthermore, individuals with psychiatric disorders often present with autonomic nervous system dysfunction, with a predominance of the sympathetic nervous system (responsible for the “fight or flight” response). This results in increased heart rate, high blood pressure, and increased vascular reactivity – factors that favour damage to arterial walls and the onset of the atherosclerotic process.
Another important factor is behaviour. Mental illness can interfere with the adoption of healthy habits. People with depression or psychotic disorders are more likely to be sedentary, have an unhealthy diet, smoke, and neglect treatment for chronic diseases. Furthermore, social isolation, common in these conditions, can increase cardiovascular risk. These patients often face barriers to accessing healthcare, which contributes to late or inadequate diagnosis of physical illnesses.
In turn, some psychotropic medications, such as certain antipsychotics and antidepressants, can also interfere with metabolism, promoting weight gain, insulin resistance, and changes in the lipid profile, which together further increase the risk of atherosclerosis.
However, it is important to emphasize that appropriate treatment of mental illness can indeed reduce these risks. Patients who receive regular psychiatric follow-up, adhere to their medication, and adopt a healthier lifestyle are less likely to develop cardiovascular complications. A collaborative approach between psychiatry and internal medicine or cardiology is essential to ensure integrated and effective treatment.
Medicine increasingly recognizes that mind and body are deeply interconnected. Mental health cannot be viewed as separate from the rest of the body. Investing in prevention, early diagnosis, and treatment of mental disorders is also a powerful way to prevent serious physical diseases, such as atherosclerosis. In short, understanding the relationship between mental illness and atherosclerosis helps not only demystify psychiatric conditions but also promote a more holistic view of health – where caring for the mind also means caring for the heart.
Article submitted by the HPA Health Group.